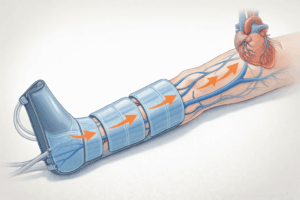
If you are managing lymphedema, you have probably seen compression boots marketed as a home recovery tool and wondered whether the same devices athletes use for sore legs could help with your condition. The answer is nuanced: pneumatic compression has a long clinical history in lymphedema treatment, but consumer recovery boots and medical-grade pneumatic compression devices are not the same thing, and using the wrong protocol can make symptoms worse.
Here is what the clinical research supports, where consumer boots fit into the picture, and the critical distinctions your lymphedema therapist will want you to understand before you plug in a device at home.
What Lymphedema Is and Why Compression Helps
Lymphedema occurs when the lymphatic system fails to adequately drain fluid from tissue, causing persistent swelling, most commonly in the arms or legs. It can be primary (caused by congenital malformation of the lymphatic vessels) or secondary (caused by damage to the lymphatic system from surgery, radiation, infection, or trauma). Secondary lymphedema is far more common, with breast cancer-related lymphedema being one of the most studied forms.
The lymphatic system has no central pump. Unlike the cardiovascular system, which has the heart, lymphatic fluid relies on muscle contractions, breathing, and external pressure to keep moving. When the lymphatic vessels are damaged or blocked, fluid accumulates in the tissue, causing swelling, heaviness, tightness, and in advanced stages, fibrotic skin changes.
Compression therapy addresses the mechanical problem directly. By applying external pressure to the affected limb, it forces interstitial fluid back into functioning lymphatic channels and into the venous system for clearance. This is the same principle behind compression bandaging, compression garments, and manual lymphatic drainage (MLD), all of which form the core of standard lymphedema treatment.
Intermittent pneumatic compression (IPC) adds a sequential, dynamic dimension to that external pressure. Instead of static squeeze, the device inflates chambers from the foot upward in a wave-like pattern, actively pumping fluid in the direction of drainage. This is why IPC has been used as an adjunct to lymphedema therapy for decades.
What the Clinical Research Shows
The evidence base for pneumatic compression lymphedema treatment is substantial but not without caveats. The research splits into two findings that matter for anyone considering the boots.
IPC reduces limb volume. A 2022 pilot trial published in Lymphatic Research and Biology studied 40 patients with confirmed lower-limb lymphedema (ISL stage II or III) and found that IPC produced significant volume reductions, with one treatment mode reducing distal leg volume by an average of 230 mL. A 2024 pilot study on patients preparing for lymphatic microsurgery found that adding IPC to complete decongestive therapy improved volume reduction compared to decongestive therapy alone.
Volume reductions are transient without ongoing treatment. The same 2022 study included a five-week washout period after IPC was discontinued, and both treatment groups showed significant rebound in volume, an increase of roughly 238 mL in the group using the more advanced device. This is a critical finding: IPC manages lymphedema actively but does not cure it, and the benefit requires regular, consistent use.
A 2025 systematic review and meta-analysis covering 14 randomized controlled trials and 1,397 breast cancer patients found that IPC significantly reduced the incidence of lymphedema when used preventively after surgery. However, its therapeutic efficacy for established, chronic lymphedema was inconsistent, with benefits observed only under specific conditions. The review recommended early intervention at pressures of 40 mmHg or below for prevention, with combined therapies needed for existing lymphedema.
Medical-Grade IPC vs Consumer Compression Boots
This is the most important distinction in this entire article, and it is the one most marketing glosses over.
Medical-grade pneumatic compression devices (Lympha Press, Bio Compression, FlexiTouch) are FDA-cleared Class II medical devices specifically designed for lymphedema. They typically feature 12 or more overlapping chambers, precise pressure calibration, specialized treatment modes that mimic manual lymphatic drainage patterns, and the ability to treat the trunk (chest, abdomen) in addition to the limb. They cost $3,000 to $8,000 and are often covered by insurance with a prescription and documentation of failed conservative therapy.
Consumer recovery boots (Normatec, Therabody RecoveryAir, Fit King, Rapid Reboot) are designed for athletic recovery. They typically have 4 to 7 chambers, simpler sequential inflation patterns, pressure ranges of 30 to 110 mmHg, and cover the legs only. They cost $200 to $1,500 and are not FDA-cleared for lymphedema treatment.
The core mechanism is the same: sequential pneumatic compression that moves fluid upward. But the clinical nuances matter significantly for lymphedema patients.
Chamber count and overlap matter. More chambers with overlapping coverage provide more even pressure distribution and prevent fluid from being trapped between inflated sections. Medical-grade devices address this with 12+ chambers. Consumer boots with 4 to 5 chambers have larger gaps between compression zones, which can push fluid into areas that are not yet compressed.
Trunk treatment matters for many patients. In lower-limb lymphedema, fluid pushed upward from the legs needs somewhere to go. If the pelvic and abdominal lymphatic pathways are also compromised, pushing leg fluid toward the trunk without addressing trunk drainage can worsen swelling above the compression point. Medical-grade devices often include abdominal or trunk garments. Consumer boots do not.
Pressure calibration matters. Lymphedema tissue responds differently than healthy muscle tissue. Pressures that feel fine for athletic recovery can be excessive for fibrotic lymphedema tissue and may cause damage to fragile lymphatic structures. The CADTH review noted concern about potential lymphatic structure damage from high-pressure IPC application.
When Consumer Boots May Be Appropriate
Not everyone with lymphedema needs a $5,000 medical device. There are specific situations where consumer lymphatic drainage boots may be a reasonable option, but they all share one prerequisite: your lymphedema therapist must be involved in the decision.
Mild, stable, early-stage lymphedema (ISL Stage I or early Stage II): patients with mild swelling that resolves partially with elevation and does not involve significant fibrosis may benefit from consumer boots as a supplement to their maintenance routine. The lower pressures available on these devices (50 to 70 mmHg) are within the range used in clinical trials.
Maintenance phase after intensive decongestive therapy: once your certified lymphedema therapist has brought swelling under control with bandaging, MLD, and exercise, a consumer boot used at home can help maintain volume reductions between clinic visits. This is not a replacement for professional care, it is a supplement to it.
General venous return support in patients with both lymphedema and prolonged immobility: patients who spend long hours sitting or standing and have mild lymphedema may find that the circulatory benefit of consumer boots addresses both the venous stasis and the lymphatic component simultaneously.
In all cases, start with your lymphedema therapist. They can assess your ISL stage, determine whether trunk involvement is a concern, recommend appropriate pressure settings, and identify any contraindications specific to your case.
When Consumer Boots Are Not Enough
There are clear situations where a consumer recovery boot is the wrong tool, and a medical-grade device or a different therapeutic approach is required.
ISL Stage III (lymphostatic elephantiasis): advanced lymphedema with significant fibrosis, skin changes, and massive swelling requires medical-grade devices with precise calibration, high chamber counts, and trunk treatment capability. Consumer boots do not have the specificity or pressure control required for this stage.
Lymphedema involving the trunk, pelvis, or genitals: consumer leg boots only compress the legs. If your lymphatic impairment extends above the groin, pushing fluid upward from the legs without addressing trunk drainage can worsen swelling in the abdomen, pelvis, or genitals. Medical-grade systems with trunk garments are necessary.
Active infection (cellulitis or lymphangitis): compression of any kind is contraindicated during active infection in the affected limb. The increased pressure can spread infection through the tissue.
Active deep vein thrombosis: an absolute contraindication for any pneumatic compression device, medical or consumer. The risk of dislodging a clot is too high.
Undiagnosed swelling: if you have new or worsening leg swelling and have not been evaluated by a clinician, do not self-treat with compression boots. Swelling can have vascular, cardiac, renal, or other systemic causes that compression therapy cannot address and may worsen.

How to Use Compression Boots Safely for Lymphedema
If your lymphedema therapist has cleared you for home use of a consumer device, the protocol differs from standard athletic recovery in several important ways.
Pressure should be lower than athletic recovery settings. The 2025 meta-analysis on breast cancer-related lymphedema recommended pressures at or below 40 mmHg for prevention protocols. For maintenance therapy, most lymphedema clinicians recommend 30 to 60 mmHg, significantly lower than the 60 to 80 mmHg range used for athletic recovery. Start at the lowest setting and increase only as directed by your therapist.
Sessions may be longer than athletic recovery. Clinical lymphedema protocols typically run 30 to 60 minutes, compared to the 20 to 30 minutes used for post-workout recovery. Your therapist will specify the appropriate duration based on your stage and response.
Frequency is higher and more consistent. Unlike athletic recovery where rest days are normal, lymphedema management often requires daily sessions to maintain volume reductions. The rebound effect shown in the clinical trials means skipping days allows fluid to re-accumulate.
Wear compression garments after the boot session. This is critical. The boots move fluid out of the tissue, but without a compression garment to maintain the reduced volume, fluid returns quickly. Always put on your compression garment immediately after removing the boots.
Monitor the limb during and after each session. Watch for increased swelling above the compression area (trunk, groin, abdomen), skin color changes, increased pain, or any signs of infection. Stop immediately and contact your therapist if any of these occur.
Insurance Coverage and Cost Considerations
For patients with documented lymphedema who have failed conservative therapy (compression garments, bandaging, exercise, skin care), medical-grade pneumatic compression devices are often covered by insurance, including Medicare. Coverage typically requires a prescription from a physician, documentation of failed conservative treatment, and sometimes prior authorization.
Consumer recovery boots are not covered by insurance for lymphedema treatment because they are not FDA-cleared for that indication. However, some consumer devices are HSA/FSA eligible, which can offset part of the cost. If your lymphedema requires IPC therapy, explore medical-grade options first, as insurance coverage can reduce your out-of-pocket cost below what a premium consumer boot would cost retail.
The Lymphology Association of North America (LANA) and the American Venous Forum both include IPC as part of consensus treatment recommendations for lymphedema, which supports insurance justification.
Compression Boots for Lymphedema, Frequently Asked Questions
Can I use Normatec boots for lymphedema?
You can, but only with your lymphedema therapist’s guidance. Normatec devices are designed for athletic recovery, not lymphedema treatment. They lack the chamber count, trunk coverage, and MLD-mimicking modes found in medical-grade devices. For mild, stable lymphedema in maintenance phase, they may serve as a supplement to your existing routine at low pressure settings. They are not a substitute for proper lymphedema therapy.
What pressure should compression boots be set at for lymphedema?
Clinical guidelines generally recommend 30 to 60 mmHg for lymphedema maintenance, which is significantly lower than the 60 to 80 mmHg range used for athletic recovery. The 2025 meta-analysis on breast cancer-related lymphedema suggested pressures at or below 40 mmHg for preventive protocols. Higher pressures risk damaging fragile lymphatic structures. Always follow your therapist’s specific recommendation.
How often should I use compression boots for lymphedema?
Daily sessions are standard for lymphedema management. The clinical evidence shows that volume reductions rebound when IPC is discontinued, meaning consistent use is essential to maintain benefit. Most protocols call for one session of 30 to 60 minutes daily, followed immediately by putting on compression garments.
Will compression boots cure my lymphedema?
No. There is no cure for lymphedema. Pneumatic compression is a management tool that reduces symptoms, specifically limb volume, heaviness, and tightness, for as long as it is used consistently. Stopping treatment allows fluid to re-accumulate. The condition requires lifelong management including compression garments, exercise, skin care, and periodic professional therapy.
Can compression boots make lymphedema worse?
Yes, if used incorrectly. Too much pressure can damage fragile lymphatic structures. Compressing the legs without addressing trunk drainage can push fluid into the abdomen or genitals. Using compression during active infection (cellulitis) can spread the infection. Using the boots without medical guidance on an undiagnosed swollen limb can mask a serious underlying condition. This is why therapist involvement is non-negotiable.
What is the difference between a lymphedema pump and compression boots?
A lymphedema pump is a medical-grade device with 12+ chambers, calibrated pressure, MLD-mimicking modes, and often trunk garments. It is FDA-cleared for lymphedema treatment and typically covered by insurance. Consumer compression boots have 4 to 7 chambers, simpler modes, and are designed for athletic recovery. The core mechanism is similar, but the clinical specificity and safety features differ significantly.
Should I see a lymphedema therapist before buying compression boots?
Yes, without exception. A certified lymphedema therapist (CLT) can assess your ISL stage, determine whether trunk involvement is a concern, identify contraindications, recommend appropriate equipment, and set pressure and duration parameters specific to your condition. Self-prescribing pneumatic compression for lymphedema without professional evaluation is where patients run into problems.
The Bottom Line
Pneumatic compression has a legitimate, evidence-backed role in lymphedema management. The mechanism is well established, the volume reductions are measurable, and the clinical research supports IPC as an effective adjunct to complete decongestive therapy.
But consumer compression boots are not interchangeable with medical-grade lymphedema devices. They can serve as a maintenance supplement for mild, stable lymphedema under therapist supervision. They cannot replace proper lymphedema therapy, treat advanced stages, or address trunk involvement.
Start with your lymphedema therapist, not with a product page. Get a proper assessment, explore insurance-covered medical-grade options first, and only consider consumer boots if your clinician specifically recommends them for your situation.