Of all the claimed benefits of compression boots, the effect on circulation is the one with the strongest scientific footing. Pneumatic compression was not invented for athletes or wellness marketing. It was developed in vascular medicine for patients with compromised blood flow, and the venous return mechanism has been studied in clinical trials for over four decades.
The short answer is yes, compression boots measurably increase blood flow velocity in the lower limbs. The longer answer matters more, because how much that increased flow helps you depends on why your circulation is sluggish in the first place.
Here is what the research actually shows, who benefits most, and where the marketing outpaces the evidence.
How Compression Boots Improve Circulation
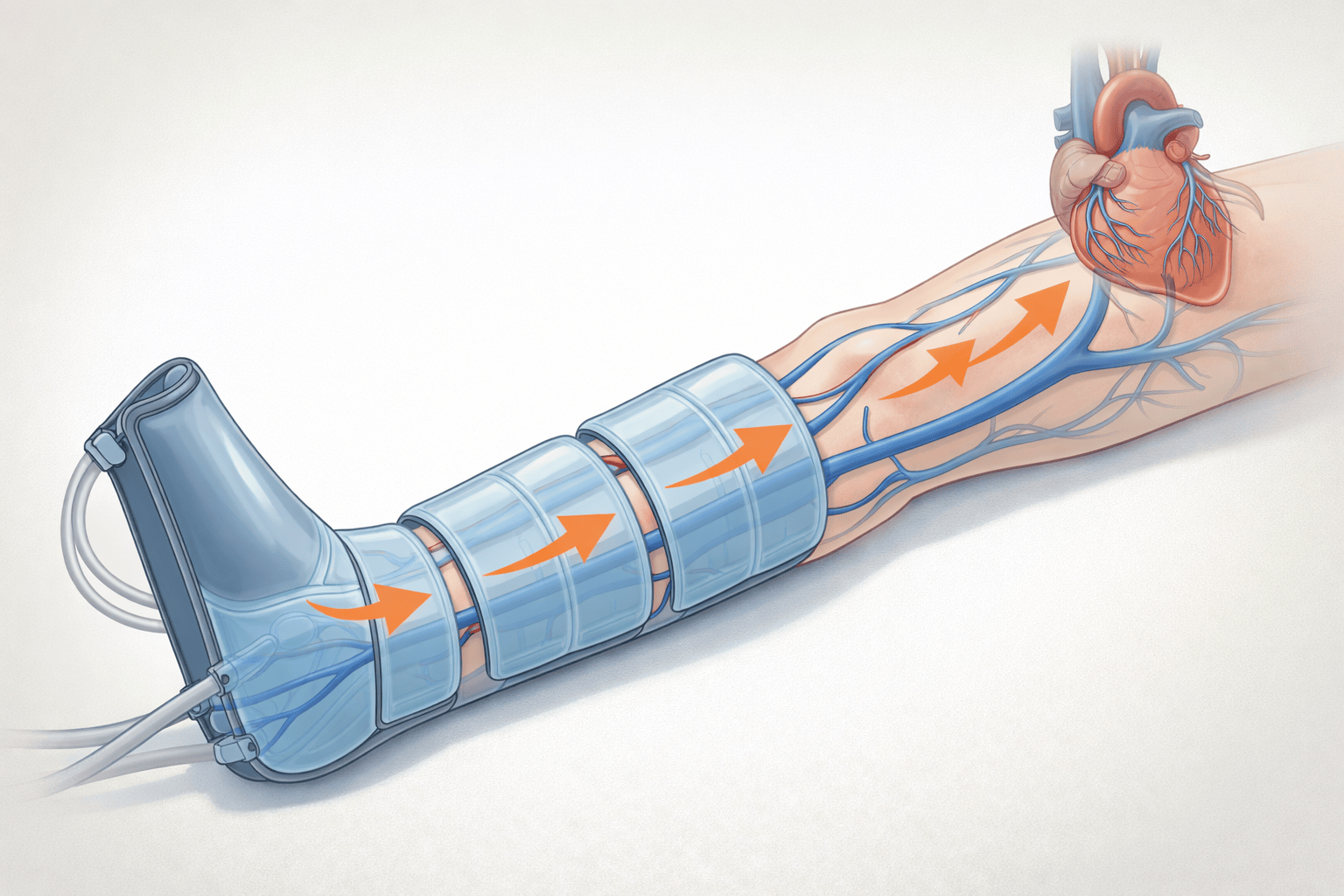
Compression boots use a technique called intermittent pneumatic compression (IPC). Air chambers inside the sleeve inflate sequentially from the foot upward through the calf, knee, and thigh, then deflate and repeat. The pressures typically run from 30 mmHg up to 100+ mmHg, depending on the device and setting.
This sequential squeeze mimics the action of the calf muscle pump, the body’s primary mechanism for pushing venous blood upward against gravity and back toward the heart. When you walk, your calf muscles contract and compress the deep veins, forcing blood upward through one-way valves. When you sit, stand still, or sleep, that pump slows dramatically. The boots do the mechanical work the calf muscles normally perform.
The effect is not theoretical. Doppler ultrasound studies have directly measured the blood flow changes during IPC. An early but influential study evaluating six different pneumatic compression devices found that the best-performing devices increased femoral venous blood flow velocity by over 200% compared to resting baseline. A 2016 randomized controlled trial on women with varicose veins found that six weeks of sequential pneumatic compression therapy significantly improved both maximum and mean venous blood velocities compared to exercise alone.
A 2026 pilot study published in Scientific Reports tested varying IPC parameters in healthy volunteers simulating immobility and found that even moderate compression at 30 mmHg produced a 90% increase in peak systolic velocity in the common femoral vein, with consistent augmentation across all participants.
What “Improved Circulation” Actually Means
The phrase “improved circulation” gets used so loosely in wellness marketing that it has almost lost meaning. It helps to be specific about what the boots actually change in the circulatory system.
Venous return velocity increases during compression. The boots push blood from the lower extremities back toward the heart faster than passive rest allows. This is the primary, best-documented effect, and it is the same mechanism hospitals use to prevent deep vein thrombosis in immobilized patients.
Arterial inflow indirectly increases. As venous blood is cleared from the limb more efficiently, the pressure differential encourages fresh, oxygenated arterial blood to flow in. This is a secondary effect, not directly driven by the compression, but it is a measurable consequence of improved venous drainage.
Lymphatic drainage is mechanically assisted. The lymphatic system runs roughly parallel to the venous system but operates at much lower pressures and lacks a central pump. The sequential compression from the boots helps move lymphatic fluid upward, reducing tissue edema and puffiness. This is the mechanism behind IPC’s long-established use in lymphedema management.
What the boots do not do: they do not permanently improve your resting circulation. They do not strengthen your veins. They do not repair damaged valves. They do not “detoxify” your bloodstream. The circulatory benefit is acute and session-dependent, meaning it happens while you are wearing them and dissipates within hours. Consistent daily use produces consistent daily benefit, but the effect does not compound into a permanent physiological change.
Who Sees the Most Circulatory Benefit
The leg compression circulation benefit is real for everyone, but the size of that benefit varies dramatically depending on your starting point. People with genuinely impaired circulation see the biggest difference.
People who stand for 8+ hours a day. Nurses, retail workers, hospitality staff, teachers, chefs. Standing immobile defeats the calf muscle pump and causes venous pooling, ankle swelling, and the heavy, aching legs that come with them. Twenty minutes in the boots after a long shift replaces the venous return work your muscles could not do all day. This is one of the clearest practical use cases for compression boots, and the benefit is immediate and noticeable.
People who sit for 8+ hours a day. Desk workers, drivers, frequent flyers. Sitting compresses the popliteal vein behind the knee and slows venous return in a different pattern than standing, but the outcome is similar: pooled blood, puffy ankles, heavy legs. The boots address this directly.
Athletes after hard lower-body training. Exercise increases blood flow to working muscles, but when you stop moving and sit down to recover, the elevated metabolic demand in the legs faces reduced venous return. The boots bridge that gap by keeping blood moving during the post-workout window when the body is transitioning from active to rest mode.
People with diagnosed venous insufficiency or mild varicose veins (with medical clearance). IPC has been used in clinical vascular medicine for exactly these conditions for decades. The 2016 randomized trial on varicose veins showed that sequential compression therapy produced significant improvements in blood flow velocity, pain reduction, and quality of life over a six-week treatment period.
Post-surgical patients (with physician guidance). Preventing DVT through mechanical compression is standard care after many surgical procedures, and the mechanism is the same one consumer compression boots use. However, post-surgical use requires medical supervision for pressure settings and session timing.
The Difference Between Compression Boots and Compression Socks
This question comes up constantly, and the answer is not “one is better.” They do different things to the same system.
Compression socks apply static, constant pressure, typically in the 15 to 30 mmHg range. They are designed to be worn during activity or extended periods of sitting and standing, and they work by reducing vein diameter so blood velocity increases passively. They prevent pooling from happening in the first place.
Compression boots apply dynamic, sequential pressure in the 30 to 100+ mmHg range. They are designed for short, focused sessions of 20 to 30 minutes, and they actively pump blood upward through the sequential inflation pattern. They clear pooling that has already happened.
The two are complementary. Wearing compression socks during a long flight prevents some of the venous stasis from occurring. Running a 20 minute boot session after landing clears whatever pooling happened despite the socks. Most people who benefit from pneumatic compression blood flow enhancement also benefit from compression socks, and vice versa.
What the Research Says About Circulation in Healthy Athletes
This is where the picture gets more nuanced. The venous return effect is real in everyone, but healthy, active athletes already have efficient circulatory systems, so the marginal gain from compression boots is smaller than it is for sedentary or standing-all-day populations.
A 2024 meta-analysis in Biology of Sport, covering 17 studies and 319 athletes, found that IPC produced measurable subjective recovery benefits but only trivial to small effects on objective physiological markers. The circulatory improvement exists, but it does not translate as clearly into measurable performance changes as the marketing implies.
A 2018 study from the University of Waterloo published in the Journal of Applied Physiology demonstrated that IPC enhanced muscle blood flow during plantar flexion exercise and recovery, confirming the acute circulatory effect exists even in healthy, exercising individuals. But the practical significance of that increased flow for recovery is where the research gets murky.
The honest framing is this: for athletes, the boots improve the sensation of circulatory recovery (lighter legs, less heaviness, less swelling) more consistently than they change measurable performance markers. Whether that subjective improvement is worth the device cost depends on your training volume and recovery needs.
Circulation Conditions That Benefit From Compression Therapy
Beyond athletic recovery, IPC has established clinical applications for specific circulatory conditions. The mechanism is the same, but the protocols and evidence base are different.
Deep vein thrombosis prevention: this is the original clinical use case for IPC, and the evidence is extensive. Systematic reviews consistently confirm that intermittent compression reduces DVT risk in immobilized patients. Consumer compression boots are not FDA-cleared for DVT prevention, but the underlying mechanism is identical to clinical-grade devices.
Chronic venous insufficiency: impaired venous return from damaged valves leads to pooling, swelling, and in severe cases, skin changes and ulceration. IPC has been shown to improve venous pump function and reduce edema in these patients, though it requires medical supervision and specific pressure protocols.
Lymphedema: IPC is a well-established complementary treatment for lymphedema, particularly in the lower limbs. A 2014 study in Lymphatic Research and Biology confirmed long-term clinical benefit from consistent IPC use in lower-limb lymphedema patients.
Peripheral artery disease (caution required): some research suggests IPC can increase arterial inflow and improve walking distance in patients with intermittent claudication, but this is a more complex clinical picture. Compression boots should only be used for PAD under direct vascular specialist supervision, as the wrong pressure settings can worsen symptoms.
Optimal Protocol for Circulatory Benefit
If you are using compression boots primarily for leg compression circulation rather than athletic soreness, the protocol shifts slightly from the standard recovery recommendations.
Pressure: 50 to 70 mmHg. Circulatory benefit does not require the higher pressures used for deep muscle recovery. The 2026 pilot study found significant venous velocity increases at just 30 mmHg, so moderate pressure is both effective and comfortable for daily venous return sessions.
Duration: 20 to 30 minutes. The standard window applies here. Longer sessions do not produce proportionally more circulatory benefit, and the venous return effect peaks within the first 15 to 20 minutes.
Frequency: daily or near-daily. Because the circulatory effect is acute and session-dependent, consistent use matters. For people using the boots to manage chronic leg heaviness, daily evening sessions produce the most noticeable results. Skipping four days and doing a long session on the fifth is far less effective than doing 20 minutes every evening.
Timing: within an hour of activity stopping, or in the evening. For desk workers, a session when you get home addresses the venous stasis that accumulated during the workday. For athletes, a session within an hour of training captures the post-exercise circulation window.
Position: legs horizontal or slightly elevated. Gravity matters. Sitting upright in a chair with feet on the floor partially defeats the venous return effect. Lying back on a couch with legs at or above heart level gives the pump the easiest path to push blood toward the heart.

What Compression Boots Cannot Do for Circulation
Worth being explicit about, because the wellness marketing has stretched the circulation claims well past what the evidence supports.
They cannot permanently fix poor circulation. The boots produce an acute, session-dependent improvement in venous return. When you take them off, circulation returns to its baseline rate within hours. Consistent use produces consistent benefit, but the underlying vascular health does not change.
They cannot replace exercise for cardiovascular health. Walking, running, cycling, and swimming produce circulatory adaptations (stronger heart, more capillary density, better endothelial function) that no passive device can replicate. The boots are a complement to movement, not a substitute for it.
They cannot treat arterial blockages, repair venous valves, or reverse vascular disease. These are structural problems that require medical or surgical intervention. The boots manage symptoms (swelling, heaviness, stasis) but do not fix root causes.
They cannot “detoxify” blood. The lymphatic and circulatory systems do not work the way detox marketing implies. Moving blood and lymph faster does not remove toxins from the body. It helps manage fluid balance and reduce edema, which is useful, but it is not detoxification.
Compression Boots for Circulation, Frequently Asked Questions
Do compression boots actually increase blood flow?
Yes, this is the most well-documented effect of intermittent pneumatic compression. Duplex Doppler ultrasound studies consistently show increased venous blood flow velocity during IPC, with some studies reporting increases of 90% or more in peak systolic velocity. The effect is acute, measurable, and consistent across healthy volunteers, athletes, and patients with venous conditions.
Can compression boots help with cold feet or numbness?
If the cold feet or numbness is caused by venous pooling or poor venous return, compression boots can help. If it is caused by arterial insufficiency, peripheral neuropathy, or nerve compression, the boots are unlikely to address the underlying issue. Persistent cold feet or numbness warrants medical evaluation before self-treating with any compression device.
Are compression boots safe for people with varicose veins?
In many cases, yes, and the research supports a benefit. A 2016 randomized trial found that sequential pneumatic compression significantly improved venous blood flow velocity and reduced pain in women with varicose veins over six weeks. However, varicose veins are a clinical condition, and compression therapy parameters should be discussed with a vascular specialist before starting regular use.
How often should I use compression boots for circulation?
Daily or near-daily sessions of 20 to 30 minutes produce the most consistent circulatory benefit, because the effect is acute and does not carry over between days. Three to five sessions per week is a reasonable minimum. Skipping long stretches and doing a single extended session does not compensate for missed days.
Do compression boots help with swollen ankles from flying?
Yes, this is one of the clearest use cases. Long flights cause venous stasis from immobility, leading to ankle and lower-leg swelling. A 20 minute session at moderate pressure after landing helps clear the accumulated fluid and visibly reduces puffiness. Wearing compression socks during the flight and running the boots after arrival is the best combined approach.
Can compression boots replace walking for circulation?
No. Walking produces dynamic calf muscle contractions, cardiovascular conditioning, and systemic circulatory adaptations that no passive device can replicate. Compression boots supplement walking, not replace it. They are most useful for the hours when you cannot walk, such as during sedentary work, after exhausting exercise, or during air travel.
The Bottom Line
The circulatory benefit of compression boots is the most mechanistically sound and best-measured effect they produce. Venous blood flow velocity increases measurably during IPC sessions, lymphatic drainage is mechanically assisted, and the subjective sensation of lighter, less swollen legs is consistent across user groups.
That benefit is biggest for people whose circulation is already compromised by immobility, prolonged standing, venous insufficiency, or post-exercise stasis. It is smallest for healthy, active people whose circulatory systems are already functioning well. And it is always acute, never permanent, which means consistency matters more than any single session.
For the right user, this is a genuine, research-backed reason to own a pair. Just do not expect the boots to fix vascular problems they were never designed to solve, or to replace the exercise your body needs to maintain circulatory health long-term.